
In July 2022 my middle child, Teddy, was diagnosed with type-1 diabetes (T1D) at the ripe full age of seven. We’re now two years past diagnosis and I’m ready to start unpacking the story.
I’ve split this story it into 5 parts:
- Our Diagnosis (this post)
- The first 24 hours
- The first 30 days
- The first 6 months
- The first 2 years
First of all, what is T1D?
Type-1 diabetes, T1D for short, it is an auto-immune disease. White blood cells mistakenly attack a healthy pancreas until the organ fails. As a result, the body is no longer able to produce enough insulin to absorb glucose in the blood stream.
There is no prevention, there is no inherent cause, and (currently) there is no cure.
There are a variety of symptoms, but the most pertinent one is a perpetually rising blood glucose (BG) level—even if a person eats zero carbohydrates (sugar). In short, the body is unable to burn sugar for energy. This is bad.
Eventually, without intervention and external sources of insulin, the liver burns fat for energy. This process produces ketones and, left unchecked, leads to a symptom called diabetic ketoacidosis (DKA). This is bad-bad.
Our Diagnosis
At time of diagnosis, Teddy’s blood glucose (BG) value was 750 mg/dL (41.7 mmol/L for everyone on the metric system).
If you’re uninitiated, like I was, that number doesn’t mean much to you.
Let me provide some brief context:
- A perfect score is 100. Normal range is often between 80-110.
- Low BG is typically anything below 80, and anything below 40 can be dangerous.
- High BG is typically anything above 120, and anything above 300 can be dangerous.
The low-end is dangerous because a person can fall unconscious and experience seizures or coma, among other complications created by fainting.
The high-end is dangerous because it can lead to DKA and contributes to organ problems, vision problems, and more. Symptoms of high BG are mainly long-term concerns, which is less immediately scary—but far more dangerous—than low BG.
Anyway, my 7yo clocking in at a BG of 750 was very, very bad. But I didn’t know any of that yet…
How we got here
In the weeks ahead of our diagnosis, we noticed Teddy would wake up at night to use the bathroom with increasing and concerning frequency. This is a symptom of many different things, such as a urinary infection, and not specific to diabetes.
As our concerns mounted, my wife, Katie, scheduled a pediatric appointment. It was up to me to take Teddy to the pediatrician because Katie was feeling a little unwell and didn’t want to risk spreading germs to anyone else (important foreshadowing).
On the way to the pediatrician’s office, the only question on Teddy’s mind was, “Am I going to get a shot??”
Teddy, like most children, hates needles. I truthfully assured him he was not getting a shot, and that we were just getting a checkup and providing a urine sample so the doctor could make sense of things.
In a matter of minutes, the pediatrician found sugar in Teddy’s urine (bad) and told us to immediately report to our local children’s hospital emergency room. Do not stop at the front desk, do not pass Go, do not collect $200. “Go immediately to the emergency room. I’ll call ahead and let them know you’re coming.”
On the drive to the hospital, I gently broke the news to Teddy that he might get a poke at this next stop. He asked, “You mean a shot??” and I carefully explained, “No, no, not a shot… but a poke. They may need to test your blood. But also maybe not!”
He was given a finger poke as soon as we walked in and then submitted to a full battery of blood tests. Every few minutes a staff member would ask Teddy, “Are you feeling okay?” and he would answer, “Yeah, why?”
Reader, this was when I learned his BG level was 750. He should, by all other measures, be feeling terrible. Dangerously terrible.
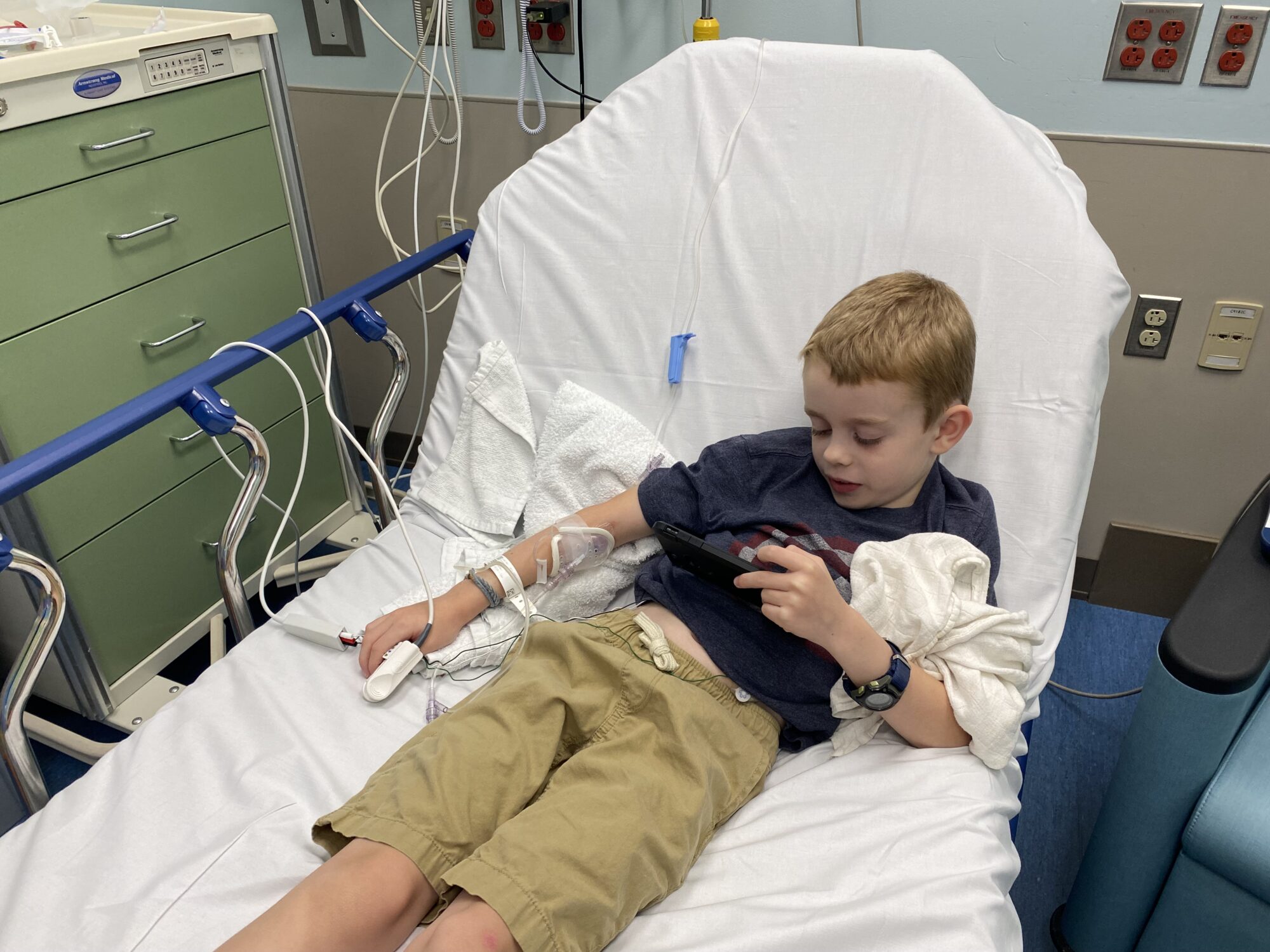
Ultimately, after a few hours in ER, we were admitted to the hospital for an overnight stay so the staff could begin administering insulin and all his vitals could be closely monitored.
Continued in: My T1D Journey: The first 24 hours
